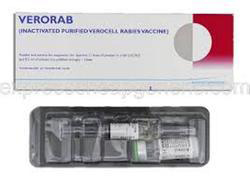
Verorab Injection 2.5 IU/ml 1 Pc
Alternative products
Rabies Vaccine [Human]
Indications
Rabies vaccine is indicated for prophylactic immunization against rabies and treatment of patients following suspected rabies contact.
Pre-exposure Immunization:
- Professional groups exposed to frequent contamination
- Veterinary surgeons (including students at veterinary colleges)
- Technical personnel working with veterinary surgeons
- Laboratory personnel handling material contaminated with rabies vims
- Personnel in abattoirs and knackers yards
- Taxidermists
- Gamekeepers, forestry workers and naturalists in enzootic areas
- Infants particularly exposed to the risk of rabies
Post-exposure Immunization:
- Treatment of subjects bitten by rabid animals or those suspected of being so
- Treatment of contact subjects.
Pharmacology
Rabies vaccine is an inactivated virus vaccine that is used for active immunisation against rabies. It can be used for pre- and post-exposure immunisation. For post-exposure immunisation, it is often used in conjunction with rabies immunoglobulins as it takes about 7-10 days for the specific antibodies to develop.
Dosage
To reconstitute the vaccine, transfer content of supplied diluent into the vial containing freeze-dried preparation. Do not shake. After reconstitution the solution should be homogeneous, clear and free from any particles. Vaccine must be injected immediately after reconstitution and the syringe should be destroyed after use.
Method of administration for intramuscular use: The 1ml dose of Rabies vaccine should be given intramuscularly in the deltoid in adults and in the anterolateral aspect of the thigh muscle in children under 1 year. It should not be injected into the gluteal region. Do not inject intravenously.
Method of administration for intradermal use: The 0.1 ml dose of Rabies vaccine (per site) should be administered intradenmally in the upper arm, over the deltoid.
Pre-exposure immunization: 1 ml for children and adults.
Primary-vaccination: According to the WHO recommendations 1 injection by the intramuscular route on days DO, D7, D21 or D28, followed by a booster dose one year later.
Boosters: Thereafter, one injection every 5 years or when the titre is found to be less than 0.5 lU/ml
Post-exposure immunization:
- Local treatment of the wound
- Vaccination of non-immunized subjects
Intramuscular schedules: One Intramuscular (IM) dose comprised of 1 ml.
Standard intramuscular (1-1-1-1-1) regimen:
- Day 0: 1 injection of 1 ml
- Day 3: 1 injection of 1 ml
- Day 7: 1 injection of 1 ml
- Day 14: 1 injection of 1 ml
- Day 28: 1 injection of 1 ml
Or
Abbreviated multisite (2-1-1) regimen:
- Day 0: 2 injections each of 1 ml at separate sites
- Day 7: 1 injection of 1 ml
- Day 21:1 injection of 1 ml
Intradermal schedules: One intradermal (ID) dose is comprised of 0.1 ml.
Thai Red Cross (2-2-2-0-1-1) schedule:
- Day 0: 2 injection each of 0.1 ml at separate sites
- Day 3: 2 injection each of 0.1 ml at separate sites
- Day 7: 2 injection each of 0.1 ml at separate sites
- Day 28: 1 injection of 0.1 ml Day 90:1 injection of 0.1 ml (optional).
Or
WHO Modified Thai Red Cross (2-2-2-0-2) schedule:
- Day 0: 2 injection each of 0.1 ml at separate sites
- Day 3: 2 injection each of 0.1 ml at separate sites
- Day 7: 2 injection each of 0.1 ml at separate sites
- Day 28: 2 injection each of 0.1 ml at separate sites
In case of severe (WHO category 3) wounds, rabies immunoglobulin should be administered as soon as possible with the first dose of rabies vaccine. The anti-rabies immunoglobulin should be used as local wound soakage injections as much as possible, with the rest part for muscle injection. The rabies vaccine should be administered in different injection site.
Vaccination of immunized subjects: If vaccine administered in less than 5 years of exposure (cell culture rabies vaccine): 2 injections one on each of DO, D3. If vaccine administered in more than 5 years of exposure or incomplete vaccination: 5 injections on DO, D3, D7, D14 and D28 with administration of immunoglobulin if required. Post-exposure vaccination must be administered on the basis of severity under medical supervision.
WHO guidelines on post-exposure treatment depending on wound severity-
Touching or feeding of animal, licks on intact skin:
- Recommended treatment: None, if reliable case history is available.
Nibbling of uncovered skin, minor scratches, superficial bites (except on head, neck, shoulder girdle.arms or hands) or abrasions without bleeding, licks on broken skin:
- Recommended treatment: Administer vaccine immediately on Day 0, D3, D7, D14 and D28.Stop treatment if animal remains healthy throughout the observation period of 10 days or if animal is killed humanely and found to be negative by appropriate laboratory techniques.
Single or multiple transdermal bites or scratches specially on head, neck, shoulder girdle,arms or hands. Contamination of mucus membrane with saliva (i.e. licks on broken skin):
- Recommended treatment: Administer rabies immunoglobulin immediately with the first dose of rabies vaccine. Administer rabies vaccine on Day 0, D3, D7, D14 and D28 or D90 (optional). Stop treatment if animal remains healthy throughout the observation period of 10 days or if animal is killed humanely and found to be negative by appropriate laboratory techniques
* চিকিৎসকের পরামর্শ মোতাবেক ঔষধ সেবন করুন'
Administration
Administrations:
- Prompt and gentle thorough washing with soap or detergent and flushing the wound with running tap water for at least 15 minutes.
- After washing, disinfectants like either ethanol (700 ml/l) or tincture or aqueous solution of iodine or povidone iodine must be applied.
- Don’t bandage or suture the wound.
Co-administration: Corticosteroid and immunosuppressive treatment may interfere with antibody production and cause vaccination failure. In these cases, a titration of neutralizing antibodies should be performed.
* চিকিৎসকের পরামর্শ মোতাবেক ঔষধ সেবন করুন'
Interaction
Concurrent use with immunosuppressants may reduce the efficacy of vaccines.
Contraindications
Rabies vaccine is contraindicated in the following cases:
Pre-exposure-
- Severe fever, febrile infection, acute disease, progressive chronic diseases
- Known hypersensitivity reactions to rabies vaccine or any of its components Post-exposure
- No contraindication to post-exposure treatment, because rabies is lethal disease, any contraindication to exposure, treatment should be considered carefully before disqualifying an individual for anti-rabies treatment.
Side Effects
Minor local reactions like pain, erythema, oedema, pruritus and induration at the injection site and lasting to 24-48 hours. Moderate fever, shivering, fainting, asthenia, dizziness, respiratory manifestations (dyspnoea, wheezing), fever, abdominal pain, vomiting and allergic skin reactions (urticaria, rash, itching).
Pregnancy & Lactation
Pregnancy. The potential risk of administration of rabies vaccine during pregnancy is unknown. Due to the severity of the disease, pregnancy is not considered to be a contraindication to post-exposure prophylaxis.
Lactation: It is not known whether the vaccine is excreted in human breast milk. Due to the severity of the disease, breast-feeding is not considered a contraindication.
Precautions & Warnings
Precaution:
- Intravenous injection is prohibited.
- The vaccine and anti-rabies immunoglobulin must not be administered with same syringe and in the same injection site.
- Before use, please carefully check package, label, appearance and the validity period.
- After reconstitution, the freeze-dried rabies vaccine should be administered as soon as possible.
- Do not shake during and after reconstitution.
Special precaution for the intradermal route:
- It is essential that intradermal administration of vaccine be administered only by medical staff trained in the ID technique in order to ensure that the vaccine is delivered intradermally and not subcutaneously.
- For the intradermal route a sterile syringe with fixed needle (insulin type) is preferred.
- A sterile needle and syringe must be used to withdraw and administer each dose of vaccine for each patient to avoid cross infection. Correct intradermal injection should result in a raised papule with a orange peel appearance. If the vaccine has been injected too deeply and a papule is not seen, the needle should be withdrawn and re-inserted nearby.
- This vaccine does not contain a preservative, therefore, great care must be taken to avoid contamination of reconstituted vaccine.
- Any reconstituted vaccine should be used as soon as possible. It must be stored in a refrigerator at +2 °C to +8 °C and used within 8 hours after reconstitution or discarded.
- ID route must not be used in the following conditions : Patient receiving immunosuppressive therapies, including irradiation, anti metabolites, alkylating agents, cytotoxic drugs and corticosteroids. Immunocompromised individuals.
Therapeutic Class
Vaccines, Anti-sera & Immunoglobulin
Reconstitution
Reconstitute with the provided diluent.
Storage Conditions
Keep out of the reach and sight of children. Store at +2 °C to +8 °C. Transportation should also be at +2 °C to +8 °C. Protect from light. Do not freeze
- Type Injection
- Tag
- Morbi leo risus
- Porta ac consectetur ac
- Vestibulum at eros