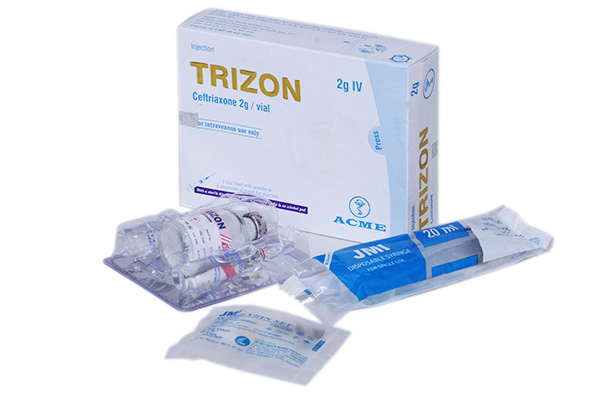
Trizon 2g IV 1 Pcs
Alternative products
Ceftriaxone
Indications
Ceftriaxone is indicated for the treatment of the following major infections:
- Lower respiratory tract infections
- Acute Bacterial Otitis Media
- Skin and skin structure infections
- Urinary tract infections
- Gonorrhea
- Bacterial Septicemia
- Bone and joint infections
- Meningitis
- Prevention of postoperative infections
- Perioperative prophylaxis of infections associated with surgery
Therapeutic Class
Third generation Cephalosporins
Pharmacology
Ceftriaxone is a 3rd generation broad-spectrum parenteral cephalosporin antibiotic. It has potent bactericidal activity against a wide range of Gram-positive and Gram-negative organisms. Like other cephalosporins and penicillins, Ceftriaxone kills bacteria by interfering with the synthesis of the bacterial cell wall. Ceftriaxone has a high degree of stability in the presence of beta lactamases. A remarkable feature of Ceftriaxone is its relatively long plasma elimination half-life of about 6 to 9 hours, which makes single or once-daily dosage of the drug appropriate for most patients. Ceftriaxone is not metabolized in the body. About 40-65% of a dose of Ceftriaxone is excreted unchanged in the urine; the remainder is excreted in the bile and ultimately found in the feces as unchanged drug and microbiologically inactive compound. The drug is highly protein bound (95%).
Dosage
Adult: The usual dose is 1 to 2 gm by intravenous or intramuscular administration once a day (or in equally divided doses twice a day).
- Pneumonia, Bronchitis, Acute bacterial otitis media, Skin and skin structure infection, Urinary tract infections, Bacterial Septicemia, Bone and joint infections, Meningitis: 1 to 2 g IV or IM once a day (or in equally divided doses twice a day); Maximum dose: 4 gm/day
- Uncomplicated gonococcal infections: 250 mg IM as a single dose
- Surgical prophylaxis: 1 g IV as a single dose 30 to 120 minutes before surgery
Infants and Children (01 month or older): The usual dose is 50 to 75 mg/kg intravenous or intramuscular administration once a day (or in equally divided doses twice a day).
- Pneumonia, Bronchitis, Skin and skin structure infection, Urinary tract infections, Bacterial Septicemia, Bone and joint infections: 50 to 75 mg/kg IV or IM once a day (or in equally divided doses twice a day); Maximum dose: 2 gm/day
- Acute bacterial otitis media: 50 mg/kg IM in single dose; Maximum dose: 1 gm/day
- Meningitis: 100 mg/kg IV or IM in single daily dose or (or in equally divided doses twice a day); Maximum dose: 4 gm/day
Duration of therapy: Continue for more than 2 days after signs and symptoms of infection have disappeared. Usual duration is 4 to 14 days; in complicated infections, longer therapy may be required.
* চিকিৎসকের পরামর্শ মোতাবেক ঔষধ সেবন করুন'
Administration
Preparation of Solutions for Intramuscular / Intravenous Injections:
- For Intramuscular Injection: 250 mg or 500 mg Ceftriaxone should be dissolved in 2 ml Lidocaine HCI 1% injection or 1 g Ceftriaxone in 3.5 ml of Lidocaine HCI 1% injection.
- For Intravenous Injection: 250 mg or 500 mg Ceftriaxone should be dissolved in 5 ml of Water for injection or 1 g Ceftriaxone in 10 ml of Water for injection USP or 2 g Ceftriaxone in 20 ml of Water for injection.
The injection should be administered over 2-4 minutes, by Intramuscular or Intravenous injection or by tubing infusion over a period of 30 minutes at concentration between 10 mg/mL and 40 mg/mL. Before starting treatment through Ceftriaxone injection, patient tolerance test should be checked by administration of a test dose. (The use of freshly reconstituted solution is recommended. However, it maintains potency for at least 6 hours at room temperature or 24 hours at 5°C).
* চিকিৎসকের পরামর্শ মোতাবেক ঔষধ সেবন করুন'
Interaction
No drug interactions have been reported.
Contraindications
Ceftriaxone should not be given to patients with a history of hypersensitivity to cephalosporin antibiotics.
Side Effects
Ceftriaxone is generally well tolerated. A few side effects such as gastro-intestinal effects including diarrhea, nausea and vomiting, stomatitis and glossitis; cutaneous reactions including rash, pruritus, urticaria, edema and erythema multiforme; hematologic reactions including eosinophilia, thrombocytopenia, leucopenia, anemia and neutropenia; hepatic reactions including elevations of SGOT or SGPT, bilirubinemia; CNS reactions including nervousness, confusion, sleep disturbances, headache, hyperactivity, convulsion, hypertonia and dizziness were reported. Local phlebitis occurs rarely following intravenous administration but can be minimized by slow injections over 2-4 minutes.
Pregnancy & Lactation
Its safety in human pregnancy has not been established. Therefore, it should not be used in pregnancy unless absolutely indicated. Low concentrations of Ceftriaxone are excreted in human milk. Caution should be exercised when Ceftriaxone is administered to a lactating mother.
Precautions & Warnings
As with other cephalosporins, anaphylactic shock cannot be ruled out even if a thorough patient history is taken. Anaphylactic shock requires immediate countermeasures such as intravenous epinephrine followed by a glucocorticoid. In rare cases, shadows suggesting sludge have been detected by sonograms of the gallbladder. This condition was reversible on discontinuation or completion of Ceftriaxone therapy. Even if such findings are associated with pain, conservative, nonsurgical management is recommended. During prolonged treatment the blood picture should be checked at regular intervals.
Use in Special Populations
Ceftriaxone must not be given to neonates if the neonates is premature and newborn (up to 28 days of age).
Overdose Effects
There is no specific antidote. Treatment of overdosage should be symptomatic.
Storage Conditions
Vial store in a cool, dry place (below 30° C), away from light & moisture. Keep out of the reach of children.
- Type Injection
- Tag
- Morbi leo risus
- Porta ac consectetur ac
- Vestibulum at eros